Hospital therapy service teams up with AFC Bournemouth for 'Sports Say' event

University Hospitals Dorset's children's therapy service has teamed up with AFC Bournemouth for an exciting, inclusive taster sports session which also aims to get feedback on how the trust can improve its services.
Suitable for all ages and abilities, the sports taster session will include adapted football and multi-sports run by AFC Bournemouth and will give young people the perfect opportunity to try out some activities and get to know others with physical disabilities. It will take place from 10am-1pm on Thursday 19 August at St Edward's School in Poole.
While the activities are taking place, parents will have the opportunity to talk with the hospital team to give feedback on the services and ways to improve.
Senior paediatric therapist, Sarah Lund, said: "We are really excited to work with AFC Bournemouth to give young people the opportunity to access football and multi sports and to learn about sports available for all abilities. We are also looking forward to hearing from young people and their families about their experiences with children's therapy services so we can make positive change to their therapy journey."
Spaces are limited so call 0300 019 2936 or email This email address is being protected from spambots. You need JavaScript enabled to view it. to book your space!
University Hospitals Dorset research teams win awards for Covid-19 research
Research teams at University Hospitals Dorset (UHD) have been presented with the Outstanding Contribution to Covid-19 Research Award for their delivery and management of clinical trials throughout the pandemic.
These NHS priority research trials involved investigating potential treatments for Covid-19 and directly impacted patient care.
The Wessex National Institute for Health Research Clinical Research Network presented the awards, recognising the UHD research teams for the pace they adapted to working with Covid-19 safety procedures in place, and upskilled to deliver brand new treatments and medications directly to patients with the virus. Some of these treatments have now been proven to be effective in treating patients with Covid-19.
Since March 2020 the research team at Poole Hospital has recruited almost 2,000 patients for a range of research trials, including interventional treatment and drug trials and observational (data collection) studies. Meanwhile at the Royal Bournemouth Hospital, the team recruited 2,678 participants for Covid-19 treatment studies, 300 of which were specially selected for the international RECOVERY trial which looked at potential treatments for Covid.
The RECOVERY research team were also winners of the Outstanding Contribution to Covid-19 Research Award, with research nurse Rebecca Miln receiving a special individual award for her contribution.
Rebecca said: “This award feels like a metaphorical pat on the back for all of our hard work. Coming together with research colleagues who we had often not worked closely with before and ensuring that we communicated and collaborated effectively made us all feel like we were contributing to something important. We are so proud to win this award, and to show the importance of well-designed clinical trials to identify life-saving treatments.
Julie Camsooksai and Beverley Wadams, senior research nurses at Poole Hospital, added: “The UK research response to Covid-19 has been incredible and we are proud that we have been part of it. It would not have been achievable without the fantastic staff across our hospitals who are with our patients from the moment they come in to when they leave.
“For us this award represents the overwhelming generosity of our patients, families and staff. Their participation in research trials has enabled the local Dorset public to be part of this enormous contribution to combatting Covid-19.”


Hospital joins exclusive list of global heart centres of excellence
University Hospitals Dorset (UHD) has been named as one of only nine centres of excellence in the world for the treatment of a debilitating heart condition at Royal Bournemouth Hospital.
Supraventricular tachycardia (SVT) is a rapid abnormal heartbeat caused by defects in the electrical system that controls the heart’s rhythm. Patients can experience a sudden rise in heart rate from a resting rate of 60 beats per minute to more than 200, leading to breathlessness, dizziness, chest pain, a pounding heart and extreme anxiety.
Arrhythmia Alliance - a coalition of charities, patient groups, patients, carers, medical groups, and allied health professionals – has now awarded UHD ‘centre of excellence’ status, in recognition of their treatment success rates – 95 per cent of patients a permanently cured of the condition - as well as an active research programme which has seen a number of scientific papers published.
UHD joins world-renowned cardiology centres including those at London’s Royal Brompton and Harefield Hospital and Stanford University in the US, who are also on the list.
The condition is treated using a technique called catheter ablation - wires are inserted from the top of the leg and guided to the heart, enabling the detection of abnormal circuits which are then cauterised.
SVT can be frightening and incapacitating, says Dr Richard Bala, consultant in electrophysiology and clinical lead in cardiac rhythm management, based at Royal Bournemouth Hospital, part of UHD.
“It’s debilitating for sufferers,” he said. “It causes unpredictable episodes of breathlessness, chest pounding and a feeling that they are about to black out, which patients can experience anything from just a few times each year to more than once a day.”
More than 300 patients with SVT from across Dorset, west Hampshire and Wiltshire have been successfully treated over the last year after undergoing catheter ablation for the condition, and more than 95 per cent of patients are permanently cured.
Ann Blake, from Bournemouth, was treated in May this year.
“My heart problems started when I had treatment for cancer 21 years ago,” explains Ann.
“The cardiology team picked up on the fact I was experiencing episodes of fast heart rhythms in my sleep - it occurred to me that it wasn’t nightmares that had been causing me to wake up in the middle of the night with a feeling of sheer panic, it was a heart problem.
“It would come on at any time, in the shower, in front of the television, anywhere - and it was frightening. I wondered each time if it was the start of a heart attack.
“Since having the treatment I haven’t had a single episode, and I don’t have to worry about one coming on unexpectedly.
“The cardiology team at Royal Bournemouth, from start to finish and throughout Covid-19, have all been incredible.”
Dr Bala says stories like Ann’s have helped the service receive worldwide attention.
“This accreditation is a reflection of the hard work and enthusiasm of our team in providing the very best care for our patients - we are very proud.”
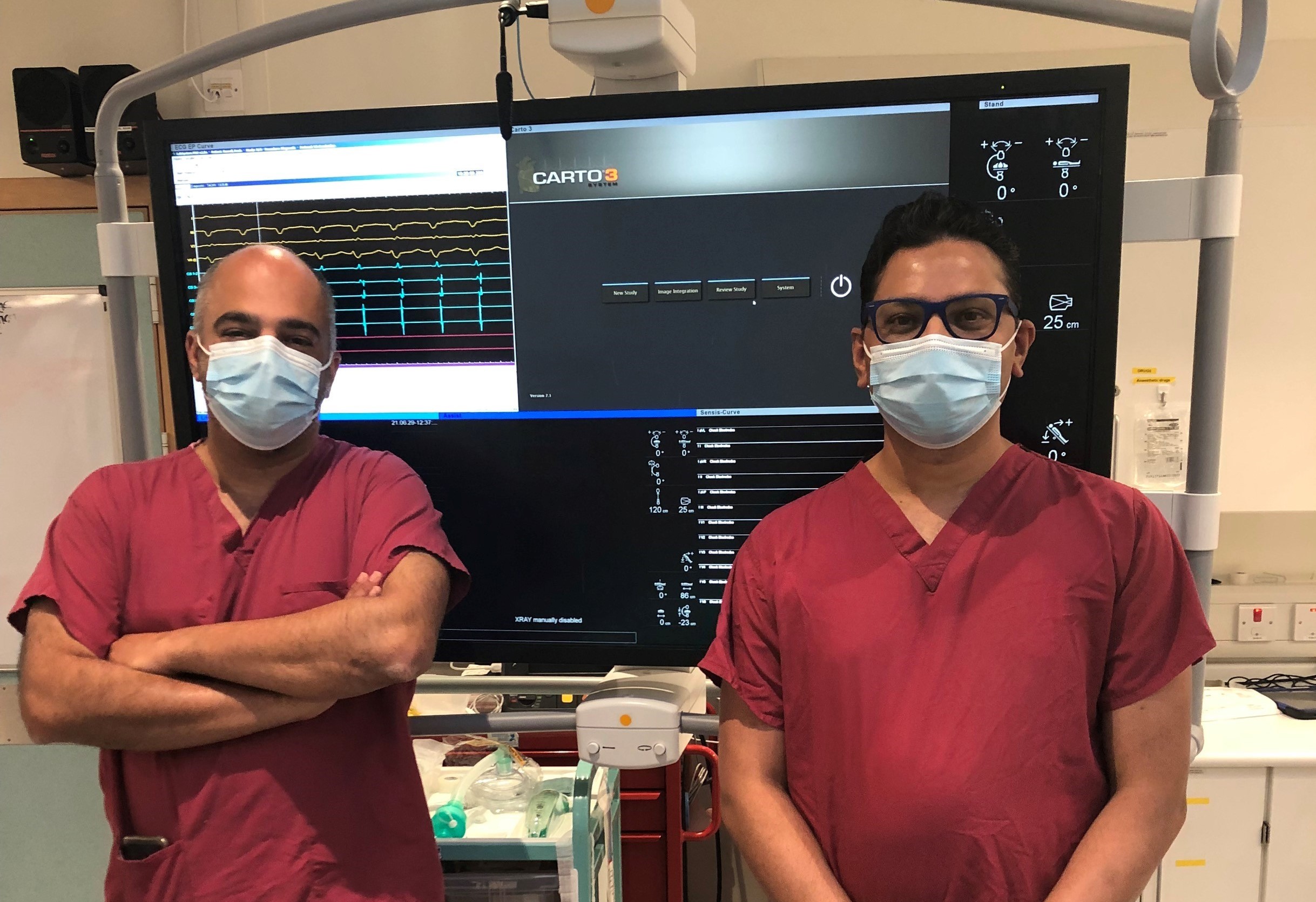
Dr Richard Bala and Dr Girish Balu, Electrophysiology Consultants
New high tech system has cancer in its sights
Cancer patients are benefiting from ultra-precise cancer treatments thanks to a new state-of-the-art system that provides clinicians with a 3D body 'map'.
University Hospitals Dorset's radiotherapy teams' two new surface-guided radiotherapy treatment systems are among only a handful available in the NHS and the first in  the south west. They use special cameras to detail the contours of a patient's skin to allow more precisely-targeted treatment during radiotherapy.
the south west. They use special cameras to detail the contours of a patient's skin to allow more precisely-targeted treatment during radiotherapy.
Radiotherapy is a procedure in which a beam of radiation is aimed at a tumour to kill it. As it can damage non-cancerous cells, the procedure involves complex planning to ensure the right dose is delivered at the exact site it is needed.
A small tattoo is typically used to denote the target site, which can remain visible after treatment and can carry its own psychological impact, which this technology will put an end to.
The high tech cameras create a skin 'map' in real time, and combined with detailed treatment planning scans previously taken, a target site is 'locked' so that if a patient – and their tumour – moves, it turns off the beam. The monitoring system is so sophisticated that it can detect movement of a fraction of a single millimetre.
The systems are being initially used to target the pelvic region, including rectal and gynaecological cancers, as well as breast cancer, before being rolled out to all cancers.
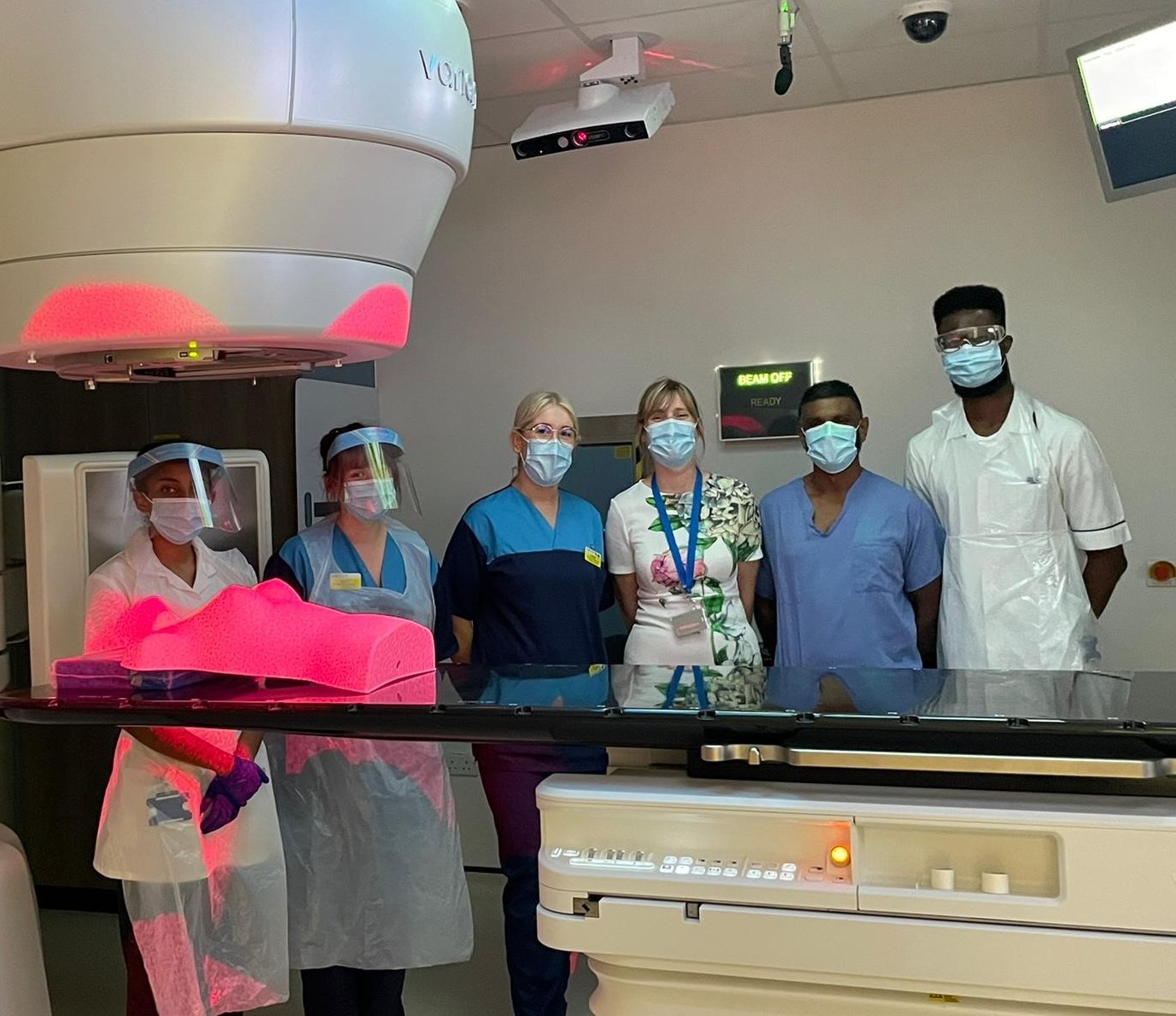 Two surface-guided systems are now in use, with a further two joining them shortly, at Poole Hospital and The Robert White Centre, at Dorset County Hospital, in Dorchester. The centre is named after multi-millionaire businessman Robert White, who gifted Poole Hospital more than £10m to advance cancer treatment in the county before his death in 2015. The Robert White Legacy Fund, a charity set up to allocate Robert's incredible legacy to appropriate projects, gave £900,000 to purchase the four systems.
Two surface-guided systems are now in use, with a further two joining them shortly, at Poole Hospital and The Robert White Centre, at Dorset County Hospital, in Dorchester. The centre is named after multi-millionaire businessman Robert White, who gifted Poole Hospital more than £10m to advance cancer treatment in the county before his death in 2015. The Robert White Legacy Fund, a charity set up to allocate Robert's incredible legacy to appropriate projects, gave £900,000 to purchase the four systems.
"When we're planning radiotherapy treatment, we spend many hours optimising each patient's treatment plan to achieve the correct dose of radiation to the tumour," said Josh Naylor, radiotherapy physicist at University Hospitals Dorset.
"All those calculations and precise planning rely on a patient remaining extremely still during the process, at the point they are receiving their radiotherapy.
"This is why you will see in use what can be very extensive shells, or masks, covering the whole head and neck, for example, to try to limit a patient's ability to move."
"The new technology will mean patients having to use these highly restrictive 'closed' masks and shells less and less, making it a more pleasant experience."
"This technology means we're more confident that we can deliver the treatment plan more precisely," added Josh.
"It will also eventually remove the need for a physical tattoo. Some patients, when we follow up with them, say that these marks are an unwelcome reminder of a difficult period in their lives and continues to cause them great stress, sometimes years after treatment and especially where it may be visible to others.
"Surface-guided radiotherapy is an incredible step forward for us, and I'm delighted that not only are we one of a handful of NHS radiotherapy services using this technology today in the UK, but that it has been made possible by Robert White and the incredible Robert White Legacy Fund to further cancer care in the county." 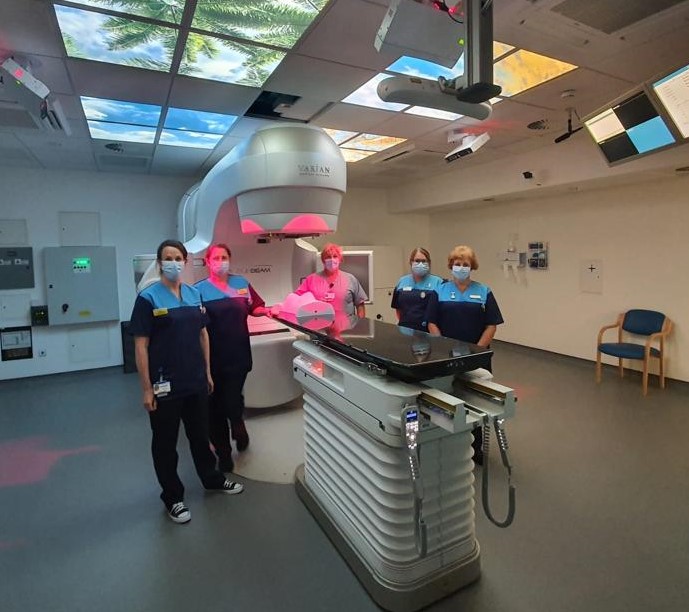
For more information on The Robert White Legacy Fund visit www.poolehospitalcharity.co.uk/robert-white-legacy-fund/.
‘Busy weekend’ for the development of UHD
The next stage of the major development around University Hospitals Dorset begins over the weekend of 30 July to 2 August leading to new access plans at Royal Bournemouth Hospital and temporary road closures at the Poole Hospital site.
The transformation works are part of a major reorganisation of services across the county which will see Royal Bournemouth Hospital becoming the centre for emergency care, with Poole Hospital becoming the main centre for planned treatment in east Dorset – all designed to improve patient care and save lives.
At Royal Bournemouth Hospital, from 2 August new access arrangements will be in place as part of the major construction project to create the new maternity, children’s, emergency, and critical care centre on the site. From that date the current main entrance will close with a new upgraded west entrance opened as well as a new retail pharmacy and orthopaedics outpatients on site. Linked to the development, a comprehensive information campaign has been developed including an updated site map to showcase the changes.
At Poole Hospital, a small section of Longfleet Road will be closed from 30 July to 2 August to allow for the installation of a new 50m tower crane ahead of the construction of the new theatre complex. The closure has been coordinated with BCP Council’s highways department, traffic management specialists, the emergency services, and teams across the hospital to maintain the best traffic and pedestrian access as possible. Diversions will be in place for through traffic, with hospital access for ambulances and pedestrians maintained over the weekend.
Commenting on the plans for the weekend, Richard Renaut, UHD chief strategy and transformation officer said:
“This is an exciting time for University Hospitals Dorset as we start the next stage in our major transformation programme which will modernise and develop our sites so that they are fit-for-purpose for their longer-term future.
“We’re sorry for the inconvenience that the busy weekend of diversions and changes to our entrances will cause - we are working closely with our contractors and Council partners to ensure disruption is kept to an absolute minimum. “
Stuart Groom, project manager, Integrated Health Projects (IHP), the trust’s principal contractor, added:
“Starting next phase of the construction programme is an important milestone for the transformation project and we look forward to continuing our productive partnership with UHD over the coming months.”
Overall, the £250m investment is the largest commitment of healthcare funding in Dorset’s history, representing a once-in-a-generation investment towards future healthcare provision for the whole of the Dorset and surrounding areas.
The updated RBH site map can be found here: www.uhd.nhs.uk/visit/finding-your-way
The BCP Council traffic notice for Longfleet Rd can be found here: https://one.network/?tm=GB122380705
More information on UHD’s future plans can be found here: www.uhd.nhs.uk/about-us/future









